# HFW-005: Claim Tracking
| Workflow Maturity | 
Newly Defined
- Workflow is defined and ARB approved
- Initial implementations are underway
|
| --------------------------- | ------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------------ |
| Description | This workflow allows a PoS to request the current processing status of a claim in the FIS. |
| Example | A hospital has sent an electronic reimbursement claim to the insurance company. After a waiting period the hospital wants to verify if the claim was processed. |
| Status | OHIE LEVEL 0 |
| Referenced Standards | HL7 FHIR Financial Module: |
| Assumptions & Prerequisites | - Unique claim identifier is managed by FIS
- The PoS system has already sent a claim to the FIS and has received a unique identifier for the claim (-> HFW-004)
|
| Actors | - PoS - The point of service system that has formulated a claim and waits for a response from the FIS.
- IOL - Mediates the transactions between the PoS system and the infrastructure services to facilitate easier interoperability.
- FIS - Financing and Insurance System that manages the claims processing and scrutinisation.
- EXT - an (OpenHIE) external payment layer
|
| Validations | The PoS or IOL should validate the FHIR resources being submitted. |
### Interaction Description
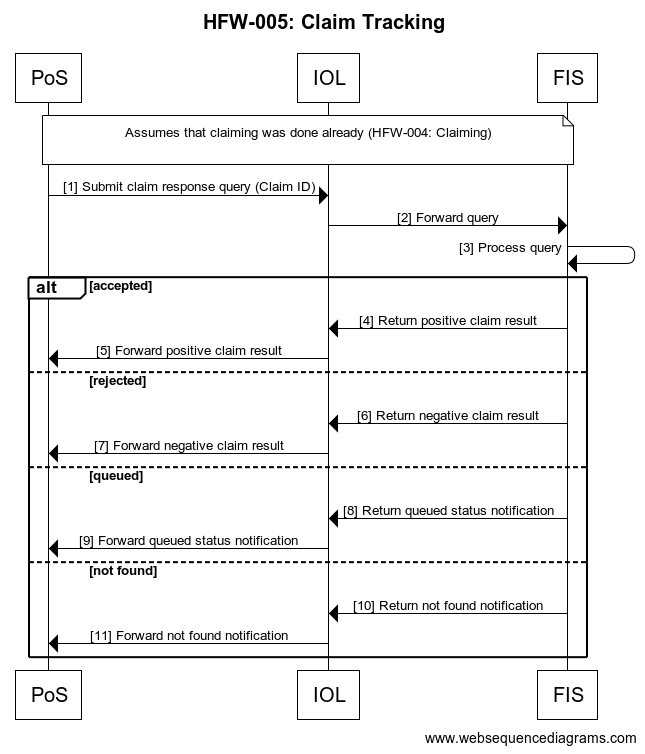
#### Source Code
(link to permanent text in [https://www.websequencediagrams.com/](https://www.websequencediagrams.com))
```
title HFW-005: Claim Tracking
participant PoS
participant IOL
participant FIS
note over PoS, FIS
Assumes that claiming was done already (HFW-004: Claiming)
end note
PoS -> IOL: [1] Submit claim response query (Claim ID)
IOL -> FIS: [2] Forward query
FIS -> FIS: [3] Process query
alt accepted
FIS -> IOL: [4] Return positive claim result
IOL -> PoS: [5] Forward positive claim result
else rejected
FIS -> IOL: [6] Return negative claim result
IOL -> PoS: [7] Forward negative claim result
else queued
FIS -> IOL: [8] Return queued status notification
IOL -> PoS: [9] Forward queued status notification
else not found
FIS -> IOL: [10] Return not found notification
IOL -> PoS: [11] Forward not found notification
end
```
### Technical Details
| Ref | Interaction | Endpoint | Data | Transaction Spec |
| --- | -------------------------------------- | -------- | ------------------ | --------------------------------------------------------- |
| 1 | Submit claim response query (Claim ID) | IOL | FHIR ClaimResponse | |
| 2 | Forward query | FIS | | |
| 3 | Process query | internal | | |
| 4 | Return positive claim result | IOL | FHIR ClaimResponse | |
| 5 | Forward positive claim result | PoS | | |
| 6 | Return negative claim result | IOL | FHIR ClaimResponse | |
| 7 | Forward negative claim result | PoS | | |
| 8 | Return queued status notification | IOL | FHIR ClaimResponse | |
| 9 | Forward queued status notification | PoS | | |
| 10 | Return not found notification | IOL | HTTP 404 | |
| 11 | Forward not found notification | PoS | | |
---
# Agent Instructions: Querying This Documentation
If you need additional information that is not directly available in this page, you can query the documentation dynamically by asking a question.
Perform an HTTP GET request on the current page URL with the `ask` query parameter:
```
GET https://guides.ohie.org/arch-spec/staging/introduction/openhie-finance-and-insurance-services-workflows/hfw-005-claim-tracking.md?ask=
```
The question should be specific, self-contained, and written in natural language.
The response will contain a direct answer to the question and relevant excerpts and sources from the documentation.
Use this mechanism when the answer is not explicitly present in the current page, you need clarification or additional context, or you want to retrieve related documentation sections.